Mini Innovation Challenge #2
Propose how a clinical tool or device used in the acute care setting - like the emergency department - can be modified or augmented to better deliver patient care.
Winner
Tyler Barr
Attending, Ventura County Medical Center
Emergency room providers at rural and smaller community hospitals are often tasked with transferring patients under their care to a facility with additional services or resources not available at their own hospital. Transferring a patient could be a simple task, but the current system typically requires multiple phone calls to various transfer centers, house supervisors and eventually other providers. It typically takes hours to even find an accepting physician at a facility with a bed available, let alone arrange transport to actually get the patient to the care that they need. Timely transfer of patients can be critical and transfer delays lead to significant patient morbidity for patients who need a higher level of care. Arranging patient transfers takes vital time and resources away from other patients leading to delays in their care. Transfer delays lead to frustration for providers who are unable to provide the care that their patients need.
-
Creating regional transfer centers (RETRACs) would organize transfer requests from hospitals with patients that require transfer and match them to nearby receiving hospitals that offer the services needed by patients. This would decrease the overall administrative burden in the healthcare system, reduce delays in transfer time, improve the care of other patients at these smaller centers as well as improve the satisfaction of providers. Information for each transfer request could be uploaded to the RETRACs via a web interface with a universal form, or perhaps even transferred directly to their database through EHR integration. Larger regional centers would similarly update the RETRACs regarding the availability of services and bed capacity. In this way, the RETRACs could automatically provide a match of the nearest facility that is able to care for the needs of the patient requiring transfer. A final phone call between the provider transferring the patient and the accepting provider would still be a vital step in communication before transferring a patient. Instead of spending time repeating the same request for transfer to various hospitals or hospital system specific transfer centers, ER providers can focus on providing care for patients in their department. Instead of suffering harm from delays in transfer, patients who need more services could be quickly routed to the closest available facility. Streamlining our archaic and chaotic transfer process would not only save time, but it would also save lives and it should be a priority for our healthcare system.
Runner-Up
Taylor Nichols
Attending, University of California San Francisco + Vituity
Telehealth has been an effective modality for expanding healthcare access, from clinical appointments in the outpatient setting for primary care on through specialist, as well as for inpatient monitoring, including in critical care settings. Physicians can monitor multiple ICU patients and even the ICUs in multiple hospitals simultaneously and manage patients via telehealth. Telehealth robots have been used to increase specialist access in emergency scenarios, such as with a tele-stroke neurologist for remote emergency departments where there may not be a neurologist available for multiple counties.
However, telehealth is vastly underutilized by emergency medicine groups and in the emergency department setting. There are numerous ways in which emergency departments and emergency medicine groups would benefit from establishing telehealth capabilities and making regular use of telehealth within their departments.
-
1) Teletriage, decreased wait times, and extra clinic expertise where and when it’s needed. For example, Vituity performed a two week pilot study on the use of teletriage in one emergency department and found that through the use of telehealth for the performance of a rapid medical evaluation, patients left without being seen decreased by 41% all while patient volumes increased by 16%.
2) Connecting emergency departments - for collaboration, more appropriate use of resources, and decreasing unnecessary transfers and allowing for appropriate specialist care to be delivered in the patient-optimized setting.
3) Remote emergency medicine - many rural or critical access emergency departments have difficulty recruiting physicians to work there or stay over longer term, sometimes due to the unsustainable travel constraints and hour requirements, including sometimes up to 48 or even 96 hour shifts straight. The use of telehealth in these settings can allow for expert clinical care to be available where and when it’s needed in remote settings while also allowing for more sustainable hours work by the on site clinician.
Finalist
Benjamin R. Wang
Medical Device Entrepreneur
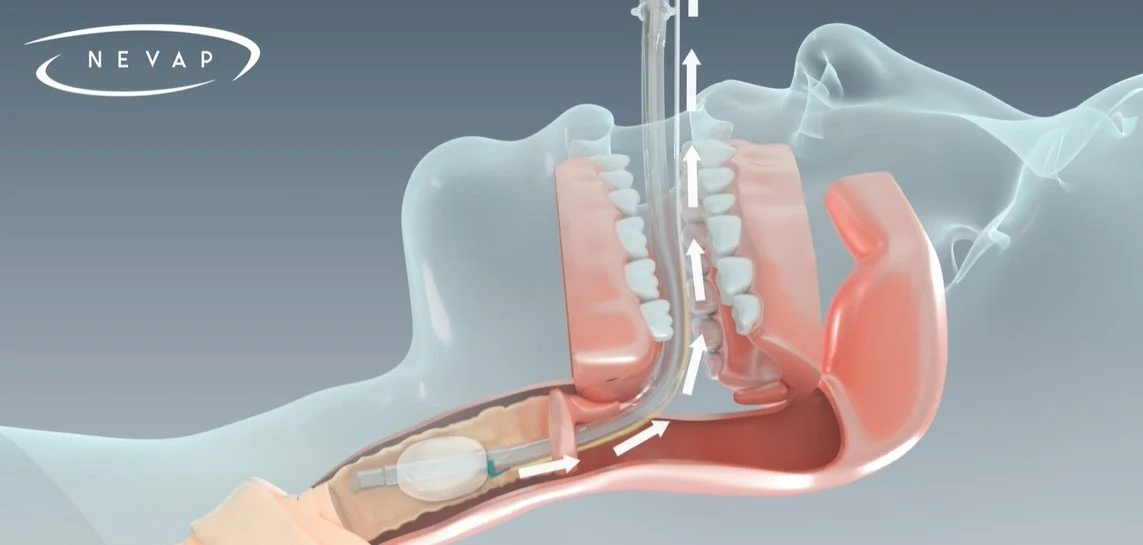
Emergency endotracheal intubation remains a high-risk procedure associated with significant per-intubation complications. Aspiration occurring during Emergency Department (ED) intubation is an unmet clinical problem leading to an 8% observed rate of aspiration pneumonia (Driver 2018). At the same time, there are no identifiable intubation factors that are correlating those patients will and will not ultimately go on to develop aspiration pneumonia (defined as any of the following in patients without a diagnosis of community acquired pneumonia, healthcare-associated pneumonia, or aspiration prior to intubation : positive sputum culture, unexplained hypoxemia, or radiographic evidence of pneumonia in the first 48hrs after intubation).
There currently is a lack of technology and protocol for the prevention of postintubation aspiration in the ED, leaving a window of time between when the patient is intubated and before an oral-gastric tube can be placed where gastric aspiration can occur. Post-aspiration, there is currently no technology or protocol in place to address fluid that accumulates below the glottis.
-
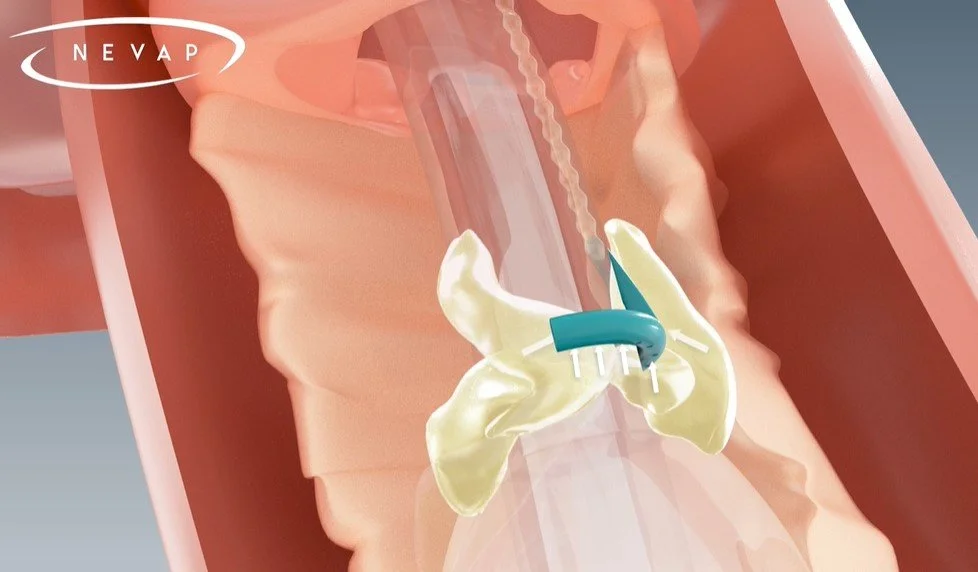
NEVAP Inc has developed an endotracheal tube with a built in channel and robust suction apparatus that can be used to quickly and reliably remove fluid that accumulates below the glottis. Utilizing this device, ED clinicians can access the airway space below the cords and drain liquid aspirate without the risk of airway trauma or occlusion by tissue/solid debris. Should the need arise, the device can be used to introduce analgesics to address the risk of increased intra-cranial pressure, and laryngospasm.